To secure your Singulair medication through insurance, confirm that your plan covers prescription medications specific to asthma and allergies. Many policies include Singulair; however, it’s crucial to review the formulary to understand any restrictions or requirements.
Prior Authorization might be necessary for some insurance plans. This means your doctor needs to provide additional information to justify the use of Singulair over other treatments. Be proactive by discussing this with your healthcare provider, ensuring all necessary documentation is prepared for submission.
If you face issues obtaining Singulair through insurance, explore patient assistance programs offered by various pharmaceutical companies. These programs can provide significant savings for eligible individuals, helping to ease the financial burden associated with medication costs.
Consider checking with your pharmacist about generic options and alternative medications that might be covered under your plan, which can further reduce out-of-pocket expenses. Understanding your insurance policy’s specific details can significantly impact access to your necessary treatments.
- Understanding Singulair Prescription Only Insurance
- What is Singulair and Its Uses in Allergy and Asthma Treatment?
- Eligibility Criteria for Singulair Prescription Coverage
- Key Criteria for Coverage
- Documentation and Submission
- How to Navigate Insurance Options for Singulair
- Potential Costs of Singulair without Insurance Coverage
- Generic Alternatives
- Discount Programs and Coupons
- Steps to Take if Your Insurance Denies Singulair Coverage
Understanding Singulair Prescription Only Insurance
To obtain Singulair through insurance, confirm that the medication is included in your plan’s formulary. This list indicates which drugs are covered. Contact your insurance provider or check their website for details.
Be prepared to provide your physician with necessary information about your insurance to ensure they can prescribe Singulair correctly. Verify whether your plan calls for a prior authorization before allowing coverage; some insurers require this step to confirm medical necessity.
Consider discussing alternative options if your insurance does not cover Singulair or if you face high copays. Generic options may provide similar benefits at a lower cost. Ask your doctor about possible alternatives that might suit your treatment plan while still being cost-effective.
Stay informed about changes in your insurance plan, as formularies can shift annually. Regularly reviewing your policy will help avoid unexpected expenses. If Singulair is excluded or restricted, digging into your options for appealing this decision could yield coverage for the medication.
Finally, explore patient assistance programs offered by drug manufacturers. These programs may provide the medication for free or at a lower cost for those without sufficient insurance coverage or financial stability.
What is Singulair and Its Uses in Allergy and Asthma Treatment?
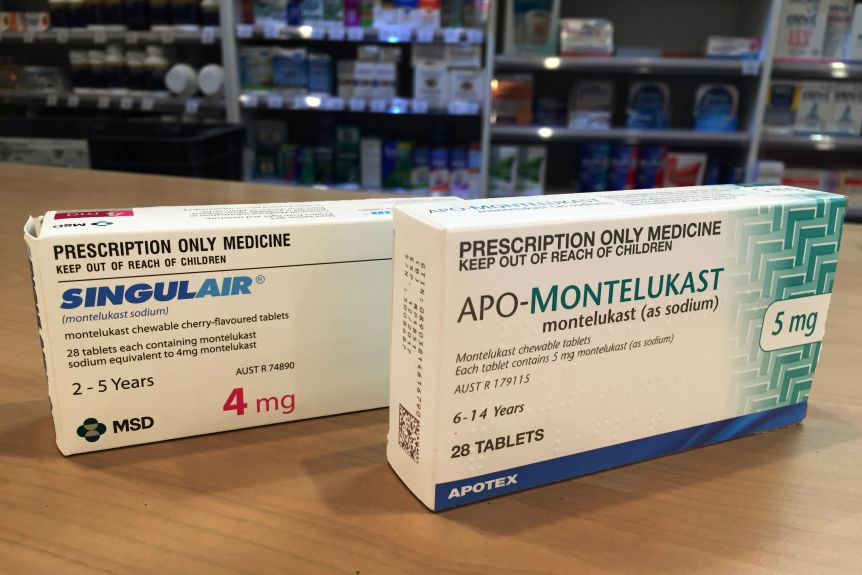
Singulair, containing montelukast, is a prescription medication commonly used for managing asthma and alleviating allergy symptoms. It blocks leukotrienes, substances in the body that cause inflammation, bronchoconstriction, and mucus production, allowing for easier breathing and reduced allergic reactions.
For asthma patients, Singulair helps prevent wheezing, shortness of breath, and nighttime symptoms. It’s particularly beneficial for those who experience exercise-induced bronchoconstriction. Taking Singulair regularly can lead to fewer asthma attacks and improved overall lung function.
In terms of allergy treatment, Singulair is effective for seasonal and perennial allergic rhinitis. It reduces symptoms such as sneezing, runny or itchy nose, and eye irritation. Patients often find they can enjoy outdoor activities with reduced discomfort.
Singulair is usually administered as a chewable tablet or a granule, making it easy for both adults and children to take. It’s important to follow the prescribed dosage to achieve optimal results. Regular consultation with a healthcare provider ensures the treatment aligns well with individual needs and any other medications being taken.
Overall, Singulair plays a crucial role in helping individuals manage asthma and allergies more effectively, leading to improved quality of life.
Eligibility Criteria for Singulair Prescription Coverage
To qualify for Singulair prescription coverage, individuals must meet specific criteria set by their insurance provider. These requirements generally include a confirmed diagnosis of asthma or allergic rhinitis along with evidence of other treatments being ineffective. Patients must typically provide documentation from their healthcare provider, indicating the necessity of Singulair for their condition.
Key Criteria for Coverage
| Criteria | Description |
|---|---|
| Diagnosis | Documentation of asthma or allergic rhinitis is required. |
| Previous Treatments | Records of previous medications and treatments that were ineffective or not tolerated. |
| Age Restrictions | Some plans have age limits for prescribing Singulair, often considering the patient’s age at the time of initial prescription. |
| Formulary Status | Singulair must be included on the insurer’s formulary list to qualify for coverage. |
| Prior Authorization | Many insurers require prior authorization to verify the need for Singulair. |
Documentation and Submission
Patients should ensure all documentation is complete before submission. It’s crucial to include a recent medical history and details of any prescribed medications. Following these guidelines significantly enhances the chances of receiving coverage approval. Keep a copy of all submitted materials for future reference.
How to Navigate Insurance Options for Singulair
Contact your insurance provider directly for specifics on coverage for Singulair. Ask about their formulary list to confirm if Singulair is included and to understand your out-of-pocket costs.
- Verify Prescription Status: Ensure that your doctor prescribes Singulair and specifies the dosage. This will help avoid any problems during the claim process.
- Check for Prior Authorization: Some plans may require prior authorization before covering Singulair. Confirm if this step is necessary to prevent delays.
- Inquire about Generic Options: Ask your insurer if they cover generic montelukast, which may offer a lower cost alternative.
- Discuss Cost-Sharing Details: Understand the co-pays, co-insurance percentages, and deductibles associated with your plan to budget effectively.
If your plan doesn’t cover Singulair, explore these alternatives:
- Ask your healthcare provider for alternative medications that might be covered.
- Look into patient assistance programs offered by the manufacturer for those without insurance or with high out-of-pocket costs.
- Consider switching to a pharmacy that may offer better prices or discounts for Singulair.
Keep records of all communications with your insurer. Document names, dates, and details to support any future claims or appeals. If you encounter issues with coverage, don’t hesitate to appeal the decision, providing all necessary documentation from your prescriber.
Lastly, reassess your insurance plan during open enrollment. Compare various plans to ensure you select one that provides optimal coverage for your specific medication needs.
Potential Costs of Singulair without Insurance Coverage
Without insurance, the cost of Singulair can reach significant amounts, affecting your budget directly. Monthly expenses for this medication can range from $250 to $400, depending on the pharmacy and location. Many patients find it difficult to keep up with these costs, especially those with chronic conditions requiring long-term treatment.
Generic Alternatives
Consider asking your healthcare provider about generic alternatives to Singulair, such as montelukast. These can offer similar benefits at a reduced price, often around $30 per month. Always consult your pharmacist to ensure you are selecting the best option for your health needs.
Discount Programs and Coupons
Many pharmaceutical companies offer discount programs or coupons that can lower costs for uninsured patients. Check the manufacturer’s website or speak with your doctor about available options to reduce expenses further. Utilizing these programs might help minimize out-of-pocket costs effectively.
Steps to Take if Your Insurance Denies Singulair Coverage
Begin by carefully reviewing your insurance company’s denial letter. Understand the specific reasons for the denial and check if it includes any errors or inaccuracies regarding your medical history or prescription details.
Next, consult with your healthcare provider. Ask them to provide documentation that supports your need for Singulair. This may include medical records, notes from your doctor, or letters detailing your treatment plan. A strong case from your physician can significantly improve your chances of obtaining coverage.
Then, contact your insurance company’s customer service department. Politely inquire about the denial and ask for clarification on their policy regarding Singulair. Having a clear understanding of their process can help you formulate a more effective appeal.
Prepare an appeal letter that addresses the reasons for the denial. Clearly state why Singulair is necessary for your condition, referencing any supporting documents from your healthcare provider. Be concise and articulate your case for why coverage should be granted.
Submit your appeal according to the guidelines provided by your insurance company. Keep copies of everything you send, and consider sending your appeal via certified mail to ensure it is received.
Allow time for your insurer to review your appeal. If you don’t receive a timely response, follow up to ensure it is being processed. Staying proactive demonstrates your commitment to obtaining the necessary treatment.
If your appeal is denied again, explore the option of an external review. Many states allow for independent reviews of insurance denials. This can provide an impartial assessment of your situation and potentially lead to a positive outcome.
Lastly, consider alternatives if coverage remains denied. Generic forms of the medication or other suitable treatments may be available. Discuss these options with your healthcare provider to ensure you continue receiving care.